What is a vein doctor called?
The official terminology for a vein doctor is “phlebologist.” The word “phlebologist” comes from “phlebology,” which is the branch of medicine concerned with the identification, diagnosis, and treatment of vascular conditions, such as spider veins, varicose veins, deep vein thrombosis, and chronic venous insufficiency.
What doctor treats vein problems?
If you have vein problems, you should visit a phlebologist, colloquially known as a vein doctor, vein specialist, vein expert, vein physician, or vascular doctor. The vein doctor should ideally have completed a residency program and fellowship in subjects related to vein care, such as minimally invasive endovascular treatments and vascular imaging.
Vein doctors can come from all fields of medicine, such as anesthesiology, dermatology, cardiology, and more. In order to become vein doctors, physicians must pass a few written examinations and tests, so the barrier to entry into phlebology is pretty low. That’s why you must consider your vein doctor’s credentials and educational background.
Inexperienced vein doctors often treat spider veins and varicose veins without diagnosing the root cause of the vein problems, leading to an increased risk of vein disease recurrence. That’s why you must find highly skilled and reliable vein doctors with specialized training in vascular imaging and minimally invasive spider vein and varicose vein treatments.
Can dermatologists treat varicose veins?
Dermatologists are medical professionals with specialized training in the diagnosis and treatment of skin conditions — not vascular or circulatory disorders. Dermatologists often provide spider vein and varicose vein treatments, but they only focus on the cosmetic aspect of the disease — not the circulatory disorder responsible for the symptoms.
Varicose veins and spider veins certainly affect your skin quality. They lead to the appearance of damaged blood vessels on your skin’s surface or bulging out of your skin, which can lead to self-consciousness and social anxiety. But they’re also symptomatic of a deeper circulatory disorder known as chronic venous insufficiency.
Dermatologists usually treat the external symptoms of venous insufficiency — spider veins and varicose veins. But they don’t have the expertise or training to treat underlying chronic venous insufficiency. Treating spider veins without addressing the root cause is like painting over a stained wall without fixing the leaking pipes — the stains (veins) will simply return.
How can I find the best vein doctors near me?
When looking for vein doctors, you must focus on your chosen physician’s credentials and educational background. Because of the low bar to entry, lots of physicians with minimal training in vein disease call themselves phlebologists. You should look for actual vein specialists, i.e., those who have undergone advanced training in the diagnosis and treatment of vein problems.
The most objective guarantor of skills and quality is board certification. The American Board of Venous and Lymphatic Medicine officially certifies the country’s top 1% of vein doctors if they pass a series of complex milestones, such as residency programs, fellowship training, and specialized training in minimally invasive vein treatments. You should look for board-certified vein doctors near your location in Maryland.
You should also go through the vein doctor’s credentials. The best vein doctors should have completed their residency programs and fellowships in a field related to vein care from reputable medical institutions. They should also have specialized training in minimally invasive spider vein and varicose vein treatments, such as radiofrequency ablation, endovenous laser ablation, venaseal, and sclerotherapy.
You should also look for friendly and compassionate vein doctors who listen to your symptoms and concerns to curate personalized vein treatment plans.
The Vein Center in Maryland is led by highly-skilled, board-certified, and Harvard-trained vein doctors who meet all of the aforementioned qualities. We individually select vein doctors from the country’s leading medical schools, residency programs, and fellowships, and most of our vein doctors are double or triple-certified. If you’re looking for a vein doctor, please schedule an appointment at our vein center in Maryland.
What happens during the first consultation?
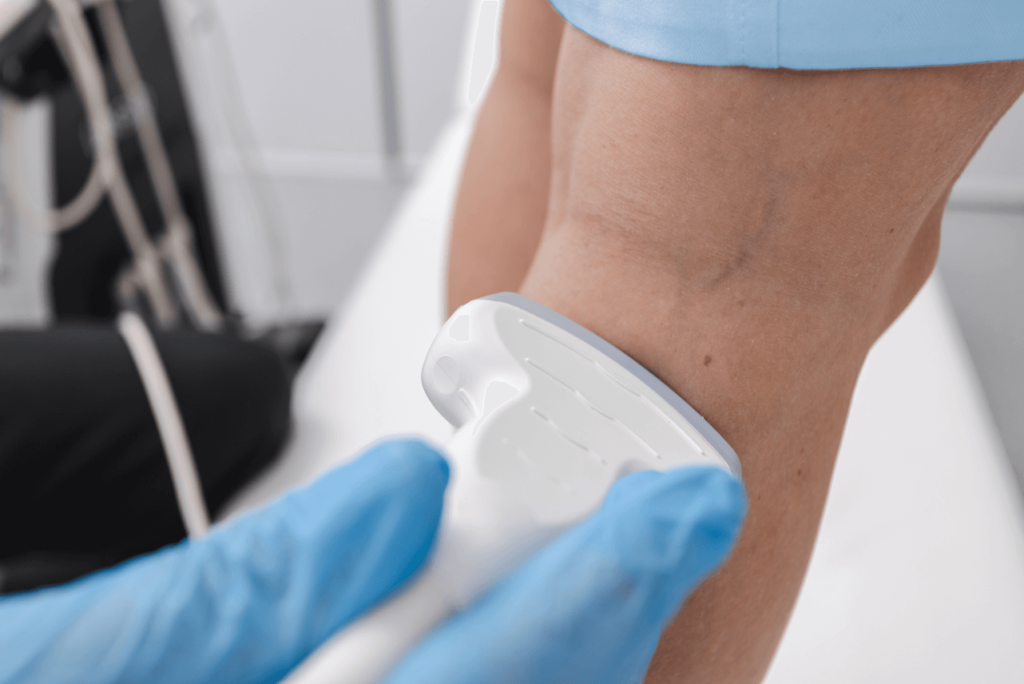
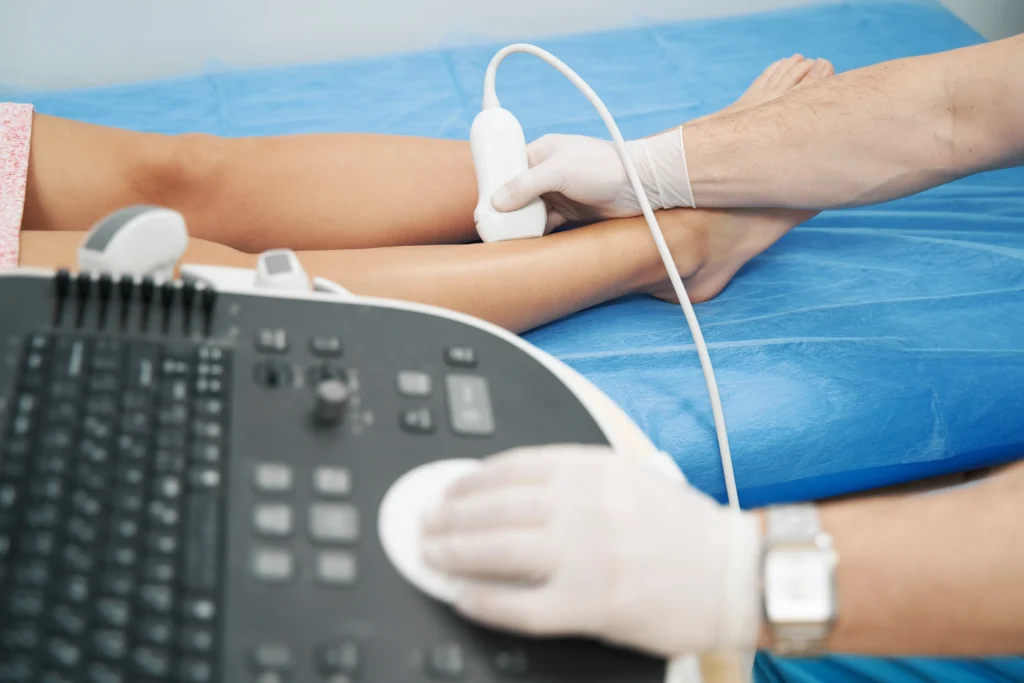
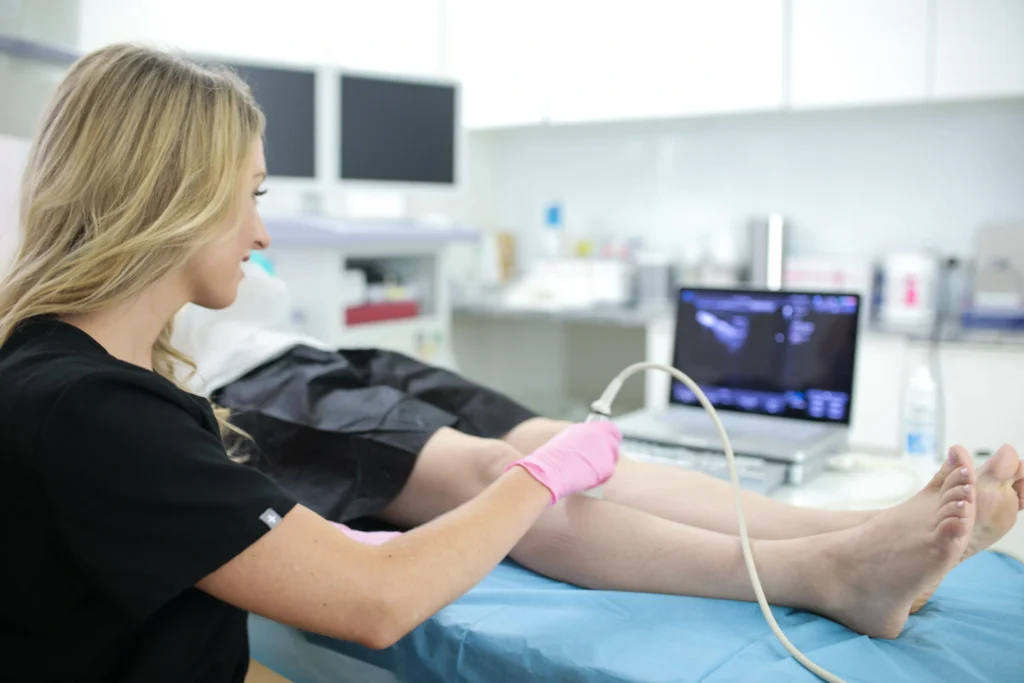
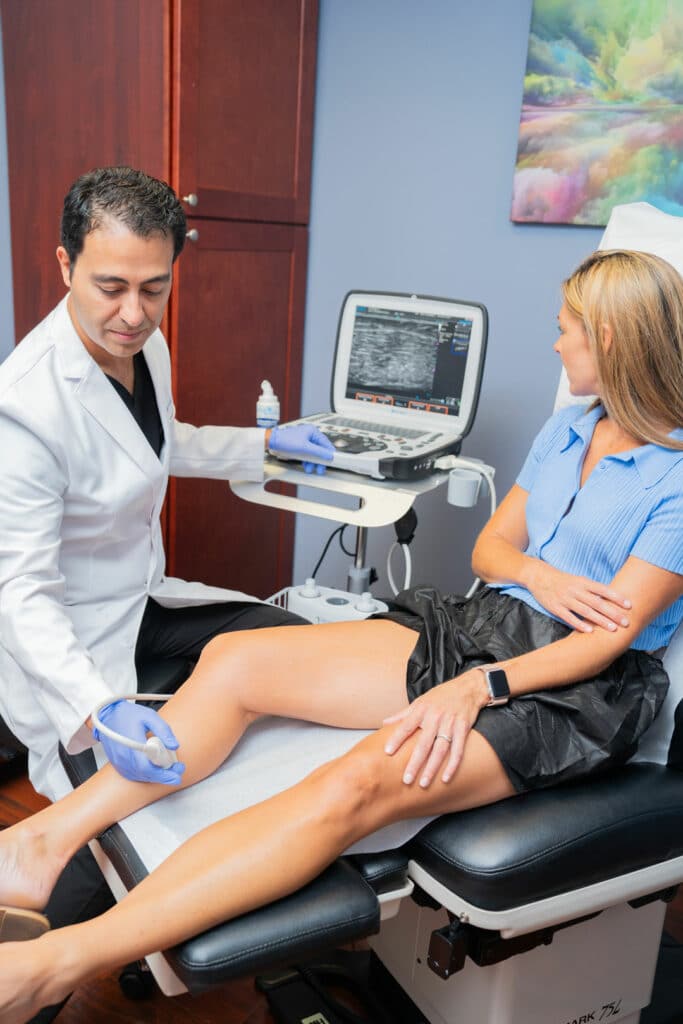
During your first consultation, the vein doctor examines your leg veins, reviews your medical history, and discusses your symptoms. The vein doctor also administers a duplex ultrasound scan, which involves channeling ultrasound energy into your legs to visualize the blood flow in your leg veins. The vein doctor interprets the results of the ultrasound test to determine if you have chronic venous insufficiency.
What is the root cause of spider veins and varicose veins?
Spider veins and varicose veins are usually caused by chronic venous insufficiency, a medical condition triggered by the collapse of vein valves. When the vein valves malfunction, gravity forces blood to flow backward (in your legs) and accumulate in the leg veins. The continued accumulation of blood in leg veins is responsible for vascular dilation and the eventual formation of spider veins and varicose veins.
What are the treatments for venous insufficiency?
Our vein center in Maryland only provides minimally invasive procedures for chronic venous insufficiency, such as radiofrequency ablation, endovenous laser ablation, and venaseal. During the vein treatment, the vein doctor channels thermal energy, laser energy, or medical adhesives into the diseased vein to destroy or seal its walls shut. The accumulated blood automatically reroutes into healthier leg veins.
What is the post-treatment recovery process?
Minimally invasive vein treatments involve minimal post-treatment side effects. You may experience mild redness, swelling, bruising, and tenderness in the treatment areas, but the risk of complications is negligible. You can also resume your daily activities and work immediately, provided you wear compression stockings and avoid strenuous workouts for a few days.