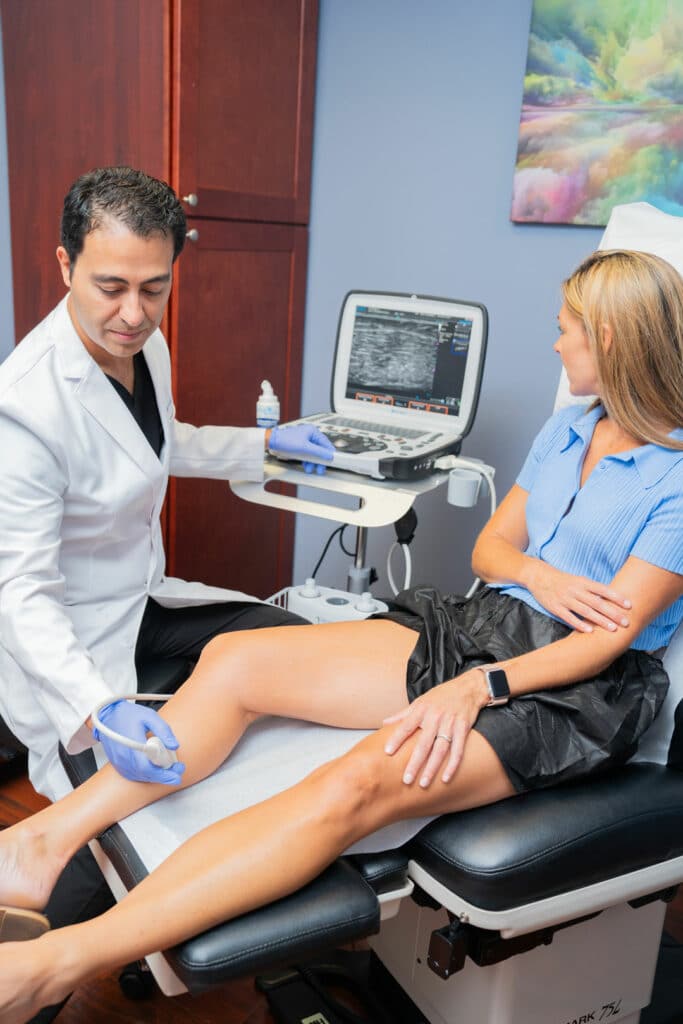
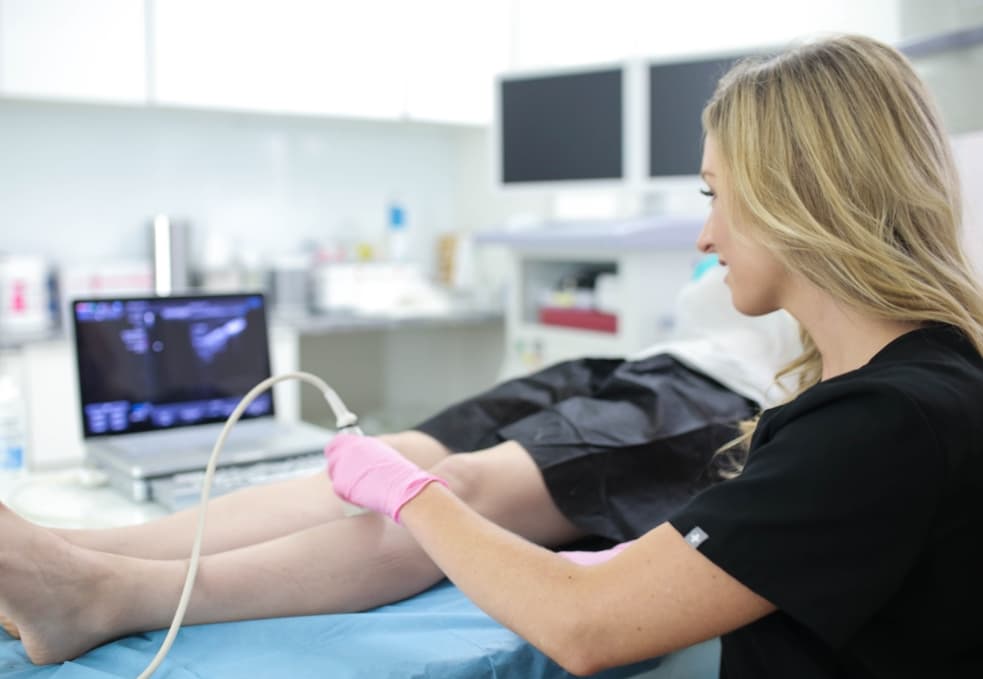
If you’ve noticed thin, web-like veins on your legs or face, commonly known as spider veins, you may wonder what causes them to appear. At Maryland Vein Center, our team of board-certified vein doctors is dedicated to providing comprehensive care for spider veins and varicose veins. In this article, we will delve into the anatomy of veins, explore the risk factors associated with spider veins, and discuss effective treatments available to you.
Understanding the Anatomy of Veins
To understand spider veins and their causes, it is crucial to have a basic knowledge of the circulatory system. Veins are an integral part of this system, responsible for carrying oxygen-depleted blood from various parts of the body back to the heart. Unlike arteries, which transport oxygen-rich blood from the heart to the body, veins work against gravity to facilitate the upward flow of blood to the heart.
To ensure efficient blood circulation, veins are equipped with one-way valves that prevent blood from flowing backward. These valves act as gatekeepers, allowing blood to move upward while restricting its backward flow. However, several factors can compromise the function of these valves, leading to the development of spider veins. When the valves become weakened or damaged, they fail to effectively regulate blood flow.
This can result in a backflow of blood, causing it to pool within the veins. The accumulation of blood exerts pressure on the vein walls, leading to spider veins and varicose veins.
Risk Factors for Spider Veins:
Several factors contribute to the development of spider veins. While some are unavoidable, understanding these risk factors can help you take preventive measures and seek timely treatment when needed.
- Age: As we age, the risk of developing spider veins increases. The natural aging process causes wear and tear on the vein walls and valves, making them more susceptible to dysfunction and the development of spider veins.
- Genetics: Family history plays a significant role in the likelihood of developing spider veins. If your parents or close relatives have spider veins or varicose veins, you may have a higher predisposition to develop them as well.
- Hormonal Changes: Hormonal fluctuations during various stages of life can contribute to the development of spider veins. Pregnancy, for example, exposes women to increased hormone levels, which can weaken vein walls and valves. Hormonal changes associated with puberty and menopause can also impact vein health.
- Obesity: Excess weight puts additional pressure on the veins, hindering proper blood flow and increasing the risk of valve dysfunction. Obesity can exacerbate the development and progression of spider veins.
- Lack of Movement: Leading a sedentary lifestyle, characterized by prolonged periods of inactivity or immobility, can contribute to poor blood circulation and increase the risk of spider veins. Regular exercise and movement help promote healthy blood flow and strengthen the muscles that support vein function.
- Hormonal Birth Control: Some forms of hormonal birth control, such as oral contraceptives or hormone replacement therapy, can increase the risk of developing spider veins. The hormonal components in these medications can impact vein health and cause dilation.
- History of Blood Clots: Individuals with a history of blood clots or deep vein thrombosis (DVT) have a higher risk of developing spider veins. Blood clots can damage vein walls and valves, leading to venous insufficiency and the formation of spider veins.
- Sun Exposure: Prolonged or excessive sun exposure can cause damage to the skin and underlying blood vessels, increasing the risk of spider veins. UV rays can weaken vein walls and contribute to their dilation.
Prevention and Lifestyle Changes
While it may not be possible to completely eliminate the risk of spider veins, certain lifestyle modifications can help reduce their occurrence or delay their progression:
- Regular Exercise: Engaging in physical activity, such as walking or swimming, promotes healthy blood flow and strengthens the muscles that support the veins.
- Maintain a Healthy Weight: Excess weight puts additional strain on the veins, increasing the likelihood of spider veins. Maintaining a healthy weight through a balanced diet and regular exercise can alleviate this risk.
- Elevate Your Legs: Elevating your legs periodically throughout the day can help reduce the pressure on the veins and improve blood flow.
- Wear Compression Stockings: Compression stockings provide graduated pressure on the legs, assisting the veins in moving blood back toward the heart. They can be particularly beneficial for individuals at higher risk of developing spider veins.
Treatment Options for Spider Veins
At Maryland Vein Center, we offer minimally invasive treatments for spider veins, tailored to your specific needs. Our board-certified vein doctors utilize advanced techniques, including:
- Sclerotherapy: This procedure involves injecting a solution into the affected veins, causing them to collapse and fade over time.
- Endovenous Laser Ablation: This technique uses laser energy to seal off problematic veins, redirecting blood flow to healthier veins.
- Radiofrequency Ablation: Similar to laser ablation, radiofrequency ablation uses heat generated by radio waves to close off diseased veins.
- VenaSeal: A medical adhesive is used to seal the affected vein, allowing blood to reroute naturally to healthier leg veins.
- ClariVein: This innovative treatment combines mechanical and chemical methods to close off the diseased veins.
- Ambulatory Phlebectomy: Small incisions are made to remove superficial varicose veins.
Visit Maryland Vein Center at Bethesda
Spider veins can be a cosmetic concern, but they can also indicate an underlying venous condition. Understanding the anatomy of veins and the risk factors associated with spider veins can help you take preventive measures and seek timely treatment when needed.
At Maryland Vein Center, our team of board-certified vein doctors is dedicated to providing personalized care and effective treatments for spider veins and varicose veins. Our vein center is conveniently located at 10215 Fernwood Rd, Suite 301, Bethesda, Maryland, just outside of Washington, DC in Silver Spring, Maryland. We offer free insurance verification to make the process seamless for our patients. Contact us for a consultation and take the first step towards healthier, more beautiful legs.